Knee osteotomy (realignment surgery)

Deciding whether to have knee surgery can feel overwhelming. This guide will help you understand your knee surgery options, benefits, risks, and recovery so you can make an informed decision about the right treatment for your condition.
-
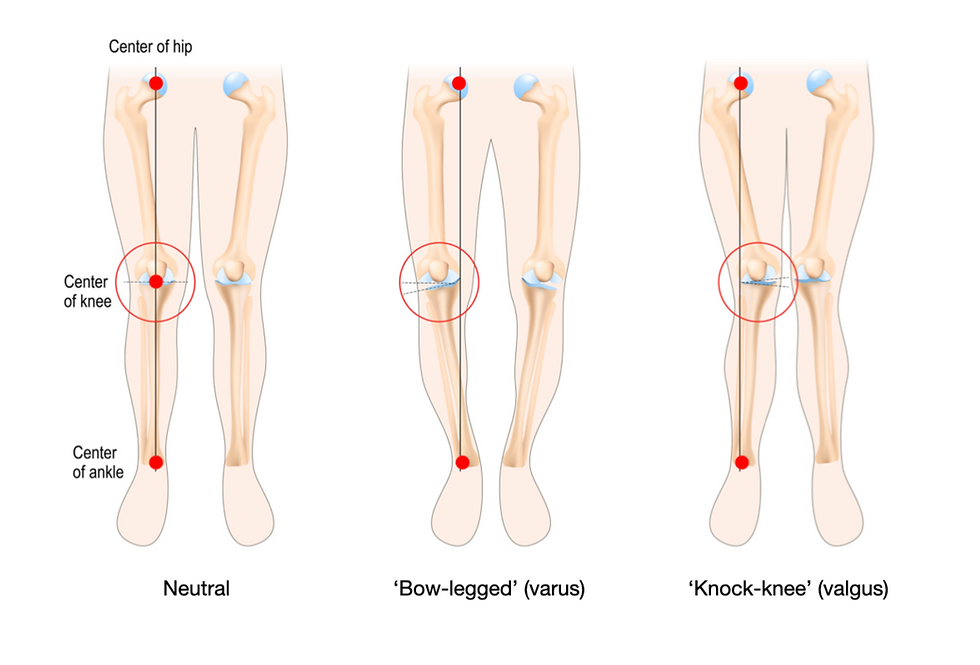
How one’s knees are aligned affects how the body weight passes through them, and can affect the mechanics of the patellofemoral (kneecap) joint.
-
If one is more ‘bow-legged’ (varus), then more of the body weight passes through the inner side of the knee (medial compartment). Likewise, if one is more ‘knock-kneed’ (valgus), more weight passes through the outer side (lateral compartment).
-
-
Knee osteotomy is performed to correct or alter the alignment of the legs. It is most commonly performed for the treatment of early arthritis, or patellofemoral instability.
-
Early Arthritis
If the body weight passes more through one side of the knee, that part can be prone to early wear (arthritis). Often the other side of the knee is relatively spared, and so realignment of the limb to move the weight bearing to the ‘good’ part of the knee can relieve symptoms (reduce pain). -
Patellofemoral (kneecap) instability
-
With significant malalignemt, the kneecap can become prone to dislocate to the side due to the malaligned pull of the muscles and tendons. Realignment surgery can correct this, and allow the kneecap to glide smoothly in the groove, preventing dislocations.
-
-
Prior to considering surgical reconstruction, patients must complete a course of physiotherapy to strengthen the core, gluteal and quadriceps muscles that allow normal knee function.
For early arthritis due to malignant, an offloaded brace may help to correct the weight bearing through the knee. These are specialised braces rather that generic knee braces that need fitting by a professional.
Living with your symptoms, and avoiding activities that cause your instability is an option, but evidence shows that people with recurrent dislocations have a poor quality of life.
The surgery will be explained to you by Mr Smith in clinic, the alternatives, likely recovery period and any associated risks discussed. You will have a pre-operative clinic appointment to ensure that you are safe for surgery, and that there is no aspect of your health that can be optimised prior to having surgery. You will be informed at this stage when to stop any regular medications, and what time you can eat and drink until prior to the surgery.
On the day of surgery you will see Mr Smith and the anaesthetist prior to the surgery, to ensure that all questions have been addressed. The consent form will be checked with you, and the correct leg marked. You will often see a physiotherapist prior to your surgery also.
-
The procedure is usually performed under a general anaesthetic (fully asleep), with a nerve block in the thigh for pain relief.
-
You will be given antibiotics into the vein at the time of surgery to reduce the risk of infection.
-
An incision is made over the side of the knee, to allow access to the bone.
-
The correction of the bone is achieved by either removing a wedge of bone (closing wedge), or opening up a wedge shape (opening wedge) within the bone.
-
Metal wires are passed across the bone under x-ray control to plan the cut in the bone. The soft tissues, nerve and vessels are protected throughout, and the bone is divided with a saw.
-
The bone is then moved to the desired position, and fixed with a metal plate and screws.
-
The incisions are then washed with sterile water, and closed with stitch that absorbs. Adherent dressings are applied, with a bandage over the top.
-
A single bone osteotomy takes under an hour to perform, with a two level correction taking longer. It may be combined with other procedures, which will increase the surgical time.
For the majority of patients the metalwork does not cause a problem and will stay in. Some patients will experience some prominence of the metal over the shin, or an ache (especially in cold weather). Plate and screw removal can easily be performed in this case.
The metal plates are made of titanium, which, although not magnetic, may trigger walk-through metal detectors, especially in more sensitive security systems.
Newer scanners (millimetre wave or body scanners) often detect the implant visually instead of relying solely on metal detection, so alarms may be less common than in the past.
Most patients will stay in hospital for a night. This allows for good pain relief after the surgery, and allows time to be seen by the physiotherapists prior to discharge.
The first few days can be a bit uncomfortable, but you will be discharged with appropriate pain relief. The quadriceps muscles often go to sleep after the surgery, and the key to the early recovery is getting them contracting again. This will allow you to start weaning off crutches, and returning towards walking unaided. The knee will be swollen, and can remain so for a few weeks. This is normal. You will have a brace for six weeks, and may have a period of protected weight bearing.
You will be seen for a wound check at two weeks, and a follow-up clinic appointment will be arranged for 6-8 weeks following the surgery, with an x-ray to assess bone healing.
The key to successful recovery is engagement in the post-operative physiotherapy programme. This is a structured, evidence-based rehabilitation regiment that ensures that the muscles and knee control are restored after surgery, to allow you to ultimately return to activities of your choosing. This must be guided by a qualified physiotherapist. An outline of the rehabilitation timeline and goals can be found here.
Regards returning to work or studies, I advise to return when ‘no longer distracted by either the pain or pain killers’. If you have an office or home based job, this can be as early as one or two weeks. For more physically demanding jobs, return to work can take longer, but you can be provided with an appropriate fitness to work (sick) note for the period.
With regards to returning to activities, this will be dictated by how the knee is recovering with physio. The bone needs to be healed, and you muscles in the legs strong enough prior to retuning to sports. The physiotherapists will guide you through this process, but full return is usually at around six months. With regards to returning to activities, this will be dictated by how the knee is recovering with physio. Driving can normally be resumed by approximately 4 weeks. I advise you inform your car insurer prior to doing so.
Tibial tuberosity osteotomy (TTO) is generally a safe and effective procedure. However, like all surgeries, it comes with risk. Every effort will be made to minimise these risks, but to allow this it is important that you mention any health issues at the pre-operative assessment. Below is a breakdown of the risks by frequency and approximate percentages, based on medical literature and clinical studies. Mr Smith will speak to you in detail about these prior to any surgery.
RiskDescriptionPain and swellingTypical post-operative symptom; managed with medication and rest (5–10%)StiffnessReduced knee range of motion; usually improves with physiotherapy (5–10%)Wound infection (superficial)Minor infection managed with oral antibiotics (1–5%)Hardware irritationPlates or screws may become uncomfortable and require removal (5–10%)Delayed bone healingSlower than expected bone union, may prolong recovery (5–10%)NumbnessAround incision site from superficial nerve irritation (5–10%)Deep infectionSerious infection requiring surgical washout and IV antibiotics (0.1–0.5%)Blood clot (Deep vein thrombosis/Pulmonary embolus/heart attack/stroke)Clot formation due to limited mobility (0.5–1%). You may be prescribed Aspirin after the surgery to reduce this riskNon-unionFailure of bone to heal, potentially requiring further surgery (0.5–1%)Fracture extensionCrack propagating from osteotomy site; may need revision surgery (0.5–1%)Over- or under-correctionMisalignment may result in uneven weight distribution or continued symptoms (0.5–1%)Permanent nerve injuryPersistent numbness or weakness from deep nerve damage (<0.1%)Vascular injuryDamage to a blood vessel during surgery (<0.1%)Compartment syndromeIncreased pressure in leg compartments requiring emergency treatment (<0.1%)Anaesthetic complicationSevere allergic or cardiorespiratory reaction to anaesthesia (<0.1%)Hardware removalMany patients require hardware removal due to irritation (up to 30%)Progression of arthritisOsteotomy delays but does not prevent arthritis progression in most casesResidual or recurrent painSome patients continue to experience symptoms despite realignment (10–20%)Leg length discrepancyMinor differences in leg length may result, especially if healing is asymmetricNeed for future knee replacementMost patients will eventually require knee replacement (timing variable)When performed for early arthritis, the majority of patients will get improvement in their symptoms for 10-12 years. After that, they may may require replacement surgery. For patellofemoral instability, 95% of patients will have no further dislocations.
Please contact the hospital where your surgery was performed, and they will easily be able to get in contact with Mr Smith on your behalf.
-
How one’s knees are aligned affects how the body weight passes through them, and can affect the mechanics of the patellofemoral (kneecap) joint.
-
If one is more ‘bow-legged’ (varus), then more of the body weight passes through the inner side of the knee (medial compartment). Likewise, if one is more ‘knock-kneed’ (valgus), more weight passes through the outer side (lateral compartment).

-
-
Knee osteotomy is performed to correct or alter the alignment of the legs. It is most commonly performed for the treatment of early arthritis, or patellofemoral instability.
-
Early Arthritis
If the body weight passes more through one side of the knee, that part can be prone to early wear (arthritis). Often the other side of the knee is relatively spared, and so realignment of the limb to move the weight bearing to the ‘good’ part of the knee can relieve symptoms (reduce pain). -
Patellofemoral (kneecap) instability
-
With significant malalignemt, the kneecap can become prone to dislocate to the side due to the malaligned pull of the muscles and tendons. Realignment surgery can correct this, and allow the kneecap to glide smoothly in the groove, preventing dislocations.
-
-
Prior to considering surgical reconstruction, patients must complete a course of physiotherapy to strengthen the core, gluteal and quadriceps muscles that allow normal knee function.
For early arthritis due to malignant, an offloaded brace may help to correct the weight bearing through the knee. These are specialised braces rather that generic knee braces that need fitting by a professional.
Living with your symptoms, and avoiding activities that cause your instability is an option, but evidence shows that people with recurrent dislocations have a poor quality of life.
The surgery will be explained to you by Mr Smith in clinic, the alternatives, likely recovery period and any associated risks discussed. You will have a pre-operative clinic appointment to ensure that you are safe for surgery, and that there is no aspect of your health that can be optimised prior to having surgery. You will be informed at this stage when to stop any regular medications, and what time you can eat and drink until prior to the surgery.
On the day of surgery you will see Mr Smith and the anaesthetist prior to the surgery, to ensure that all questions have been addressed. The consent form will be checked with you, and the correct leg marked. You will often see a physiotherapist prior to your surgery also.
-
The procedure is usually performed under a general anaesthetic (fully asleep), with a nerve block in the thigh for pain relief.
-
You will be given antibiotics into the vein at the time of surgery to reduce the risk of infection.
-
An incision is made over the side of the knee, to allow access to the bone.
-
The correction of the bone is achieved by either removing a wedge of bone (closing wedge), or opening up a wedge shape (opening wedge) within the bone.
-
Metal wires are passed across the bone under x-ray control to plan the cut in the bone. The soft tissues, nerve and vessels are protected throughout, and the bone is divided with a saw.
-
The bone is then moved to the desired position, and fixed with a metal plate and screws.
-
The incisions are then washed with sterile water, and closed with stitch that absorbs. Adherent dressings are applied, with a bandage over the top.
-
A single bone osteotomy takes under an hour to perform, with a two level correction taking longer. It may be combined with other procedures, which will increase the surgical time.
For the majority of patients the metalwork does not cause a problem and will stay in. Some patients will experience some prominence of the metal over the shin, or an ache (especially in cold weather). Plate and screw removal can easily be performed in this case.
The metal plates are made of titanium, which, although not magnetic, may trigger walk-through metal detectors, especially in more sensitive security systems.
Newer scanners (millimetre wave or body scanners) often detect the implant visually instead of relying solely on metal detection, so alarms may be less common than in the past.
Most patients will stay in hospital for a night. This allows for good pain relief after the surgery, and allows time to be seen by the physiotherapists prior to discharge.
The first few days can be a bit uncomfortable, but you will be discharged with appropriate pain relief. The quadriceps muscles often go to sleep after the surgery, and the key to the early recovery is getting them contracting again. This will allow you to start weaning off crutches, and returning towards walking unaided. The knee will be swollen, and can remain so for a few weeks. This is normal. You will have a brace for six weeks, and may have a period of protected weight bearing.
You will be seen for a wound check at two weeks, and a follow-up clinic appointment will be arranged for 6-8 weeks following the surgery, with an x-ray to assess bone healing.
The key to successful recovery is engagement in the post-operative physiotherapy programme. This is a structured, evidence-based rehabilitation regiment that ensures that the muscles and knee control are restored after surgery, to allow you to ultimately return to activities of your choosing. This must be guided by a qualified physiotherapist. An outline of the rehabilitation timeline and goals can be found here.
Regards returning to work or studies, I advise to return when ‘no longer distracted by either the pain or pain killers’. If you have an office or home based job, this can be as early as one or two weeks. For more physically demanding jobs, return to work can take longer, but you can be provided with an appropriate fitness to work (sick) note for the period.
With regards to returning to activities, this will be dictated by how the knee is recovering with physio. The bone needs to be healed, and you muscles in the legs strong enough prior to retuning to sports. The physiotherapists will guide you through this process, but full return is usually at around six months. With regards to returning to activities, this will be dictated by how the knee is recovering with physio. Driving can normally be resumed by approximately 4 weeks. I advise you inform your car insurer prior to doing so.
Tibial tuberosity osteotomy (TTO) is generally a safe and effective procedure. However, like all surgeries, it comes with risk. Every effort will be made to minimise these risks, but to allow this it is important that you mention any health issues at the pre-operative assessment. Below is a breakdown of the risks by frequency and approximate percentages, based on medical literature and clinical studies. Mr Smith will speak to you in detail about these prior to any surgery.
RiskDescriptionPain and swellingTypical post-operative symptom; managed with medication and rest (5–10%)StiffnessReduced knee range of motion; usually improves with physiotherapy (5–10%)Wound infection (superficial)Minor infection managed with oral antibiotics (1–5%)Hardware irritationPlates or screws may become uncomfortable and require removal (5–10%)Delayed bone healingSlower than expected bone union, may prolong recovery (5–10%)NumbnessAround incision site from superficial nerve irritation (5–10%)Deep infectionSerious infection requiring surgical washout and IV antibiotics (0.1–0.5%)Blood clot (Deep vein thrombosis/Pulmonary embolus/heart attack/stroke)Clot formation due to limited mobility (0.5–1%). You may be prescribed Aspirin after the surgery to reduce this riskNon-unionFailure of bone to heal, potentially requiring further surgery (0.5–1%)Fracture extensionCrack propagating from osteotomy site; may need revision surgery (0.5–1%)Over- or under-correctionMisalignment may result in uneven weight distribution or continued symptoms (0.5–1%)Permanent nerve injuryPersistent numbness or weakness from deep nerve damage (<0.1%)Vascular injuryDamage to a blood vessel during surgery (<0.1%)Compartment syndromeIncreased pressure in leg compartments requiring emergency treatment (<0.1%)Anaesthetic complicationSevere allergic or cardiorespiratory reaction to anaesthesia (<0.1%)Hardware removalMany patients require hardware removal due to irritation (up to 30%)Progression of arthritisOsteotomy delays but does not prevent arthritis progression in most casesResidual or recurrent painSome patients continue to experience symptoms despite realignment (10–20%)Leg length discrepancyMinor differences in leg length may result, especially if healing is asymmetricNeed for future knee replacementMost patients will eventually require knee replacement (timing variable)When performed for early arthritis, the majority of patients will get improvement in their symptoms for 10-12 years. After that, they may may require replacement surgery. For patellofemoral instability, 95% of patients will have no further dislocations.
Please contact the hospital where your surgery was performed, and they will easily be able to get in contact with Mr Smith on your behalf.
